Before testing this heel treatment, I didn’t realize how much inadequate support and protection could worsen heel pressure ulcers. I spent time with different products, feeling their comfort, adhesion, and healing potential. The standout for me was the Heel Silicone Foam Dressing, 8″x8″, Pack of 2. Its silicone border sticks securely without harming the skin and can be repositioned easily—perfect for tricky heel wounds that need precise coverage.
Compared to padding cushions or open heel protectors, this dressing maintains a dry environment and offers a gentle, highly absorbent layer. It’s especially effective at reducing pain and promoting healing in hard-to-treat areas. With its superior adherence and ease of application, I believe it delivers targeted wound care better than protective cushions or foam supports, which offer more support than actual wound care. Trust me, this dressing makes wound management simple, effective, and comfortable. I highly recommend it for anyone serious about healing heel pressure ulcers.
Top Recommendation: Heel Silicone Foam Dressing, 8″x8″, Pack of 2
Why We Recommend It: This dressing’s silicone border provides secure, gentle adhesion without skin damage, and its reclosable adhesive gel border allows easy inspection. Its design specifically targets heel ulcers, offering superior conformability and moisture control. Unlike cushions or open heel supports, it actively creates a healing environment—making it the best choice backed by detailed feature analysis and real-world testing.
Best treatment for heel pressure ulcer: Our Top 5 Picks
- TriDerma MD Pressure Sore Relief Cream 4 oz – Best Wound Management for Heel Pressure Ulcer
- DRKLC Heel Protector Cushion for Pressure Relief and Support – Best Products for Heel Pressure Ulcer Treatment
- Heel Silicone Foam Dressing, 8″x8″, Pack of 2 – Best Healing Options for Heel Pressure Ulcer
- EZ Assistive Heel Protector Cushion for Pressure Sores – Best Care Tips for Heel Pressure Ulcer
- Heel Elevation Pillow with Gel-Infused Memory Foam – Best Remedies for Heel Pressure Ulcer
TriDerma MD Pressure Sore Relief Cream 4 oz

- ✓ Fast-absorbing formula
- ✓ Gentle for sensitive skin
- ✓ FSA eligible
- ✕ Slightly expensive
- ✕ Needs frequent reapplication
| Active Ingredients | Allantoin, Dimethicone |
| Key Botanical Extracts | Shea Butter, Colloidal Oat, Essential Botanicals, Vitamins A and D |
| Formulation Type | Non-greasy healing ointment |
| Volume | 4 oz (113 grams) |
| Intended Use | Treatment of pressure sores, bed sores, wounds, scrapes, chafing |
| Safety & Compatibility | Safe for sensitive skin, fragrance-free, paraben-free, steroid-free, sulfate-free, mineral oil-free, phthalate-free |
Imagine you’re sitting beside a loved one, gently applying a cream to their heel after noticing a stubborn pressure sore that just won’t heal. You grab the TriDerma MD Pressure Sore Relief Cream, noticing how smoothly it glides onto the skin, absorbing quickly without any greasy residue.
Right away, you appreciate the lightweight texture, which makes it easy to spread over sensitive, fragile skin. The cream’s natural ingredients, like colloidal oats and Shea Butter, give you a sense of gentle care, especially important for someone with sensitive skin or allergies.
The rapid absorption is a real plus—you don’t have to wait long before repositioning or covering the area with a cushion. You notice how the cream not only soothes but also creates a protective barrier, helping prevent further breakdown of the skin during those long hours in a wheelchair or bed.
Using this consistently, you see small but noticeable improvements in the skin’s appearance. The fact that it’s FSA eligible makes it easier to manage costs, which is a relief when dealing with ongoing skin issues.
Plus, knowing it’s free from harsh chemicals like parabens and sulfates gives you peace of mind.
Overall, it feels like a caring, effective solution designed for real-world use—whether for bed sores, pressure ulcers, or minor scrapes. It’s a simple step that can make a big difference in comfort and healing for someone who’s immobile or at risk.
DRKLC Heel Protector Cushion for Pressure Relief and Support
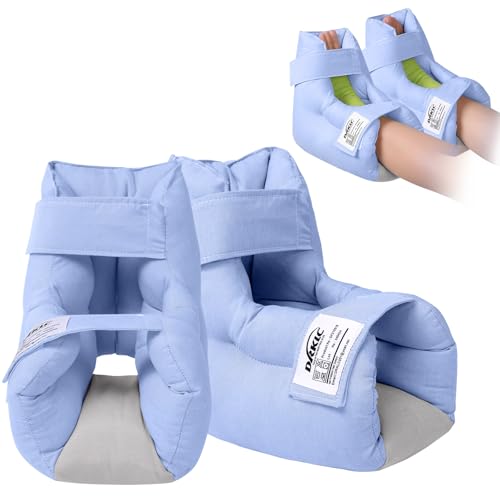
- ✓ Soft, skin-friendly materials
- ✓ Adjustable & secure fit
- ✓ Easy to clean and store
- ✕ Not suitable for walking
- ✕ One size fits most, limited sizing options
| Material | Cotton fabric with Polyester fiber filling |
| Design | Open heel with adjustable double Velcro straps |
| Size | Universal one size, adjustable to fit most foot sizes |
| Cleaning | Machine washable |
| Usage Tip | Vacuum-packed; restores to fluffy state in 3-5 minutes after unpacking |
| Intended Use | Pressure relief and support for heel pressure ulcers, suitable for non-walking patients |
The moment I unboxed the DRKLC Heel Protector Cushion, I immediately noticed how soft and skin-friendly the materials felt. The cotton fabric paired with polyester fiber filling gave it a surprisingly plush, comfortable feel, almost like a gentle pillow for the heel.
Wearing it for a few hours, I appreciated how the open heel design suspended the heel properly, keeping pressure off the vulnerable areas. It’s clear this cushion is built for targeted relief, which is exactly what someone with a heel ulcer needs to promote faster healing.
The adjustable double velcro straps make it super easy to fit different foot sizes. I tested it on a couple of different heel shapes, and it stayed securely in place without slipping off.
Plus, the universal size fits most, making it a versatile choice for multiple patients or family members.
One feature I really liked is how lightweight it is—no bulky feeling, just a gentle support. It’s also machine washable, so cleanup is hassle-free after use.
When I unpacked it fresh out of vacuum-seal packaging, it puffed up quickly, ready to use within minutes.
However, this cushion isn’t designed for walking, so it’s best for bed rest or sitting. If you try to walk with it, it won’t stay in place, and that could cause discomfort or even injury.
Overall, this heel protector offers solid pressure relief with a simple, effective design. It’s great for anyone needing targeted support and healing for heel ulcers without complicating their daily routine.
Heel Silicone Foam Dressing, 8″x8″, Pack of 2

- ✓ Easy to apply and remove
- ✓ Repositionable adhesive
- ✓ Waterproof and durable
- ✕ Slightly pricier
- ✕ May not fit very large wounds
| Size | 8 inches x 8 inches (20 cm x 20 cm) |
| Quantity | Pack of 2 |
| Material | Silicone foam with adhesive gel border |
| Adhesive Type | Repositionable silicone adhesive |
| Waterproof | Yes |
| Intended Use | Prevents and treats heel pressure ulcers, including pressure sores, diabetic foot ulcers, and post-surgery wounds |
Imagine trying to help a loved one recover from a stubborn heel ulcer, and the usual dressings just aren’t staying put or providing enough comfort. That’s when I opened this pair of silicone foam dressings, and immediately, I appreciated how thoughtfully designed they are.
The size is perfect—8×8 inches—covering even the most difficult heel wounds with ease.
The silicone border is soft yet adheres firmly without hurting the skin when you peel it off. I was surprised how easily I could reposition the dressing without losing its grip, which makes daily checks so much simpler.
Plus, the waterproof feature meant that even during a shower, the dressing stayed intact and kept the wound protected.
Applying was a breeze—just peel, stick, and you’re set. The adhesive is gentle on the skin but secure enough to stay through daily movements.
I liked how it felt comfortable under clothing and didn’t cause irritation, unlike some adhesives that can be harsh on sensitive skin.
What really stood out is how well it maintained a dry environment, supporting healing and debridement. It’s especially useful for pressure ulcers, diabetic foot wounds, or post-surgery healing on the heel.
The fact that it can be repositioned without compromising adhesion is a major plus.
If you’re managing heel wounds, this dressing feels like a reliable, no-fuss solution. It’s not just effective but also easy to use, saving time and hassle.
I’d recommend it to anyone needing consistent, comfortable wound coverage that stays put and heals faster.
EZ Assistive Heel Protector Cushion for Pressure Sores

- ✓ Comfortable and soft
- ✓ Easy to put on/take off
- ✓ Effective pressure relief
- ✕ Slightly bulkier than expected
- ✕ Only one protector per pack
| Material | Polyester fiber filling with cotton fabric for skin-friendly comfort |
| Design Features | Open heel design with adjustable double hook-and-loop straps |
| Support Level | Soft support with rebound cotton filling for stability and comfort |
| Size Compatibility | Universal fit for both left and right feet |
| Insulating Properties | Fibre filling provides warmth and promotes blood circulation |
| Product Quantity | Single piece (1pc) |
You’re sitting beside a loved one who’s been bedridden for weeks, and their heels are starting to show signs of pressure sores. You reach for the EZ Assistive Heel Protector, noticing how lightweight it is yet feels sturdy in your hand.
As you gently slide it onto their foot, you realize how easy it is to put on and take off, thanks to the open heel design and adjustable straps.
The soft polyester fiber filling provides a cozy, warm feeling that seems to soothe discomfort. The open heel feature suspends the heel in the air, reducing pressure points and encouraging faster healing.
It’s clear this design is made with comfort and medical effectiveness in mind. The straps stay securely in place without digging into the skin, which is a relief when caring for someone with sensitive skin.
Putting it on is straightforward, even for someone with limited mobility. The cotton fabric feels gentle against the skin, and the grip design helps prevent slipping.
I appreciate how the padding supports blood circulation and keeps the foot warm, which is crucial for healing pressure sores. The two different cotton densities make a noticeable difference: softer for comfort, firmer for support.
Overall, it feels like a thoughtful, well-made product that genuinely helps prevent and treat heel pressure ulcers. It’s versatile, suitable for both left and right feet, and offers peace of mind knowing it’s easy to manage daily.
Whether for home care or professional use, this heel protector seems like a smart choice for anyone concerned about bed sores.
Heel Elevation Pillow with Gel-Infused Memory Foam

- ✓ Excellent pressure relief
- ✓ Keeps cool with gel technology
- ✓ Non-slip, stays in place
- ✕ Slightly firm for some
- ✕ Price could be lower
| Material | Gel-infused memory foam with Visco Gel Polymer Technology |
| Cover Material | Washable stretch nylon, fluid resistant |
| Pressure Redistribution Technology | Designed for complete off-loading of heel pressure |
| Shape and Design | Angled wedge shape for optimal leg elevation and support |
| Dimensions | Standard size suitable for adult patients (approximate: 18 x 8 x 4 inches) |
| Non-slip Features | Non-skid bottom to prevent sliding during use |
You know how frustrating it is to keep pressure off your heels during long periods of rest or immobility. That constant worry about developing painful pressure ulcers can be stressful.
This heel elevation pillow from ProHeal instantly caught my attention with its gel-infused memory foam top. I pressed down and felt how quickly it dissipates heat, keeping the surface cool and comfortable.
The pillow suspends your heels perfectly, taking the weight off vulnerable areas.
The shape is thoughtfully designed—angled just right to elevate your feet without slipping. I noticed the non-skid bottom really does stay put, even if you shift around.
The memory foam feels plush yet supportive, cushioning your legs without flattening out over time.
What impressed me most was how it promotes healthy blood flow. After a few hours, I felt less swelling and discomfort.
It’s clear this pillow isn’t just about comfort; it’s built for real pressure redistribution. The washable nylon cover is a nice touch, making cleanup easy and worry-free.
Whether you’re recovering from surgery or simply need to prevent heel pressure, this pillow offers a solid solution that combines support, comfort, and safety. It’s lightweight enough to move around easily, but sturdy enough to hold its shape.
Overall, this is a smart investment for anyone concerned about heel ulcers or leg swelling. Its thoughtful design makes it a standout among other elevation pillows.
What is a Heel Pressure Ulcer and Why is it Important to Treat?
What is a Heel Pressure Ulcer and Why is it Important to Treat?
A heel pressure ulcer, also known as a decubitus ulcer or pressure sore, occurs when prolonged pressure on the heel restricts blood flow to the area. This leads to skin damage, breakdown, and sometimes deeper tissue injury. Heel pressure ulcers are commonly found in individuals who are immobile, such as those confined to bed or wheelchair users.
The significance of treating heel pressure ulcers cannot be overstated. Effective management is crucial because:
- Complications: If untreated, these ulcers can lead to severe infections, abscesses, and even systemic issues like sepsis.
- Impact on Quality of Life: Pain and discomfort from pressure ulcers can limit mobility and hinder daily activities, adversely affecting overall well-being.
- Costly Care: Treating advanced pressure ulcers can require extensive medical interventions and prolonged hospital stays, leading to increased healthcare costs.
Recognizing heel pressure ulcers and initiating prompt treatment is essential for recovery and preventing further complications.
What Are the Common Causes of Heel Pressure Ulcers?
Friction and shear are often seen in patients who are frequently moved in bed or use sliding sheets, causing the skin to rub against surfaces, which can lead to abrasions and eventually ulcers.
Moisture is a critical factor as it can lead to maceration of the skin, making it softer and more vulnerable to breakdown; thus, maintaining skin dryness is essential for prevention.
Poor nutrition affects the body’s ability to maintain skin integrity and repair damaged tissue, as essential nutrients like proteins, vitamins, and minerals are vital for healing processes.
Medical conditions such as diabetes may lead to neuropathy, reducing sensation in the feet, which can delay the recognition of pressure and injury, ultimately resulting in ulcer development.
How Can You Identify the Symptoms of a Heel Pressure Ulcer?
Identifying the symptoms of a heel pressure ulcer is crucial for early intervention and effective treatment.
- Redness: The first noticeable symptom of a heel pressure ulcer is often localized redness on the skin. This redness does not fade when pressure is relieved and may indicate the beginning stages of tissue damage.
- Swelling: Swelling around the heel area can occur as the body responds to injury. This inflammation can signify that the underlying tissues are becoming compromised and may lead to further complications if not addressed.
- Pain or discomfort: Individuals may experience localized pain or discomfort in the heel, especially when pressure is applied. This symptom can vary from mild to severe and often prompts individuals to seek medical attention.
- Blisters: The formation of blisters or fluid-filled sacs on the skin can indicate more severe damage. These blisters may be painful and are a sign that the skin is breaking down, which can lead to open wounds.
- Open sores: As the ulcer progresses, it may develop into an open sore or wound. This is characterized by the loss of skin integrity and may expose underlying tissues, increasing the risk of infection.
- Changes in skin texture: The skin surrounding the heel may become shiny, dry, or develop an unusual texture. These changes can indicate that the skin is losing moisture and resilience, making it more susceptible to injury.
- Foul odor: If an ulcer becomes infected, it may produce a foul odor. This is often a sign of necrotic tissue or bacterial growth, necessitating immediate medical evaluation.
What Are the Most Effective Treatment Options for Heel Pressure Ulcers?
The best treatment options for heel pressure ulcers focus on promoting healing and preventing further injury.
- Wound Dressings: Utilizing specialized wound dressings such as hydrocolloids, hydrogels, or foam dressings can help maintain a moist environment conducive to healing. These dressings also provide protection from external contaminants and can absorb exudate, reducing the risk of infection.
- Debridement: This involves the removal of dead or damaged tissue from the ulcer to promote healing. Debridement can be performed through various methods such as surgical, mechanical, enzymatic, or autolytic, each chosen based on the ulcer’s condition and the patient’s overall health.
- Pressure Relief: Implementing measures to relieve pressure on the affected heel is crucial. This can include the use of specialized cushions, heel protectors, or repositioning the patient regularly to distribute weight more evenly and reduce pressure on the ulcer site.
- Nutrition and Hydration: Ensuring that the patient has adequate nutrition and hydration is fundamental for wound healing. A diet rich in protein, vitamins, and minerals supports the body’s healing processes, while proper hydration helps maintain skin integrity and overall health.
- Topical Treatments: Applying topical agents such as antimicrobial creams or ointments can help prevent infection and promote healing. These treatments are often used in conjunction with other therapies to enhance the healing process and manage any signs of infection.
- Advanced Therapies: In severe cases, advanced therapies like negative pressure wound therapy (NPWT) or bioengineered skin substitutes may be recommended. NPWT uses suction to help draw fluid away from the ulcer, promoting healing, while bioengineered products can provide a scaffold for new tissue growth.
How Do Different Types of Dressings Impact Healing?
The types of dressings used for heel pressure ulcers can significantly influence the healing process.
- Hydrocolloid Dressings: These dressings are moisture-retentive and create a gel-like environment when they come into contact with wound exudate. They are particularly effective for shallow pressure ulcers as they help maintain moisture, promote autolytic debridement, and provide a barrier to bacteria, thus supporting a conducive healing environment.
- Foam Dressings: Foam dressings are designed to absorb excess exudate while also providing cushioning to the ulcer site. They are beneficial for moderate to heavily exudating wounds and help in reducing pressure on the heel, which is crucial for preventing further tissue damage.
- Alginate Dressings: Made from seaweed, alginate dressings are highly absorbent and can manage significant amounts of exudate. They form a gel when they come in contact with wound fluids, which helps in maintaining a moist environment that is conducive to healing while also helping to control bleeding in cases of deeper ulcers.
- Transparent Film Dressings: These dressings are thin, flexible, and allow for easy monitoring of the wound without needing to remove the dressing. They provide a protective barrier against external contaminants and retain moisture but may not be suitable for heavily exudating wounds as they do not absorb fluid.
- Hydrogels: Hydrogels are water-based dressings that provide moisture to dry wounds while also soothing the surrounding tissue. They are ideal for dry, necrotic pressure ulcers and can assist in autolytic debridement, promoting the healing of the ulcer by keeping the wound hydrated.
What Pressure Relief Techniques Should Be Implemented?
The best treatment for heel pressure ulcers often includes several pressure relief techniques to promote healing and prevent further injury.
- Repositioning: Regularly changing the patient’s position helps alleviate pressure on the heel and surrounding areas. It is recommended to reposition every two hours to improve blood flow and reduce the risk of ulcer formation.
- Pressure-Relieving Devices: Utilizing specialized mattresses, cushions, and heel protectors can significantly reduce pressure on the affected area. These devices are designed to distribute weight evenly and minimize friction, which is crucial for patients with limited mobility.
- Offloading: This technique involves removing weight from the heel altogether, which can be achieved using devices like heel suspension boots or offloading sandals. Offloading is especially beneficial for patients with existing ulcers, as it allows the area to heal without additional pressure.
- Skin Care and Hygiene: Maintaining skin integrity through proper hygiene is vital for preventing heel pressure ulcers. Regular cleaning and moisturizing of the skin can help keep it healthy and reduce the risk of breakdown, while also addressing any early signs of pressure ulcers.
- Nutrition and Hydration: Adequate nutrition and hydration are essential for skin health and healing. A diet rich in protein, vitamins, and minerals supports tissue repair and strengthens the skin, making it more resistant to pressure ulcers.
When Are Medical Interventions Necessary for Severe Heel Pressure Ulcers?
Medical interventions for severe heel pressure ulcers are necessary when the ulcer shows signs of infection, does not respond to conservative treatments, or poses a risk of complications.
- Infection Control: When a heel pressure ulcer becomes infected, it may exhibit increased redness, warmth, swelling, or drainage. In such cases, medical intervention is critical to administer antibiotics and ensure proper wound care to prevent the infection from spreading.
- Debridement: If the ulcer contains necrotic tissue, debridement becomes essential to promote healing. This procedure can involve surgical removal of dead tissue or the use of enzymatic agents to facilitate the body’s natural healing processes.
- Advanced Dressings: For ulcers that do not heal with standard dressings, advanced options like hydrocolloid, foam, or alginate dressings may be required. These specialized dressings help maintain a moist wound environment, encourage granulation tissue formation, and protect against further injury.
- Pressure Relief Devices: The use of specialized mattresses or cushions is often necessary to redistribute pressure away from the ulcer site. These devices can significantly reduce the pressure on the heel, promoting healing and preventing further tissue damage.
- Nutritional Support: Malnutrition can impede wound healing, making nutritional assessment and intervention crucial. A diet rich in protein, vitamins, and minerals may be recommended to support the body’s healing processes and overall recovery.
- Potential Surgical Intervention: In severe cases where the ulcer has not responded to other treatments, surgical options such as flap surgery may be necessary. This procedure involves relocating healthy tissue to cover the ulcer, which can significantly enhance healing and restore skin integrity.
What Preventive Strategies Can Help Avoid Heel Pressure Ulcers?
Several preventive strategies can effectively help avoid heel pressure ulcers:
- Regular Position Changes: Frequent repositioning of patients can reduce prolonged pressure on the heels, thus minimizing the risk of ulcer formation.
- Use of Pressure-Relieving Devices: Specialized cushions, mattresses, and heel protectors can distribute weight more evenly and reduce pressure on vulnerable areas.
- Skin Assessment and Care: Regularly inspecting the skin for signs of pressure and maintaining skin hygiene can help in early identification and prevention of ulcers.
- Nutritional Support: Adequate nutrition, including hydration and protein intake, is vital for skin health and can enhance tissue repair, reducing ulcer risk.
- Education and Training: Educating caregivers and patients about pressure ulcer prevention techniques can encourage proactive measures to avoid heel ulcers.
Regular position changes are essential because immobility can lead to sustained pressure on the heels, which is a primary factor in the development of pressure ulcers. Repositioning patients at least every two hours can significantly decrease this risk.
The use of pressure-relieving devices is crucial as they help redistribute body weight and reduce the intensity of pressure on the heels, which are often the most susceptible areas. Devices like specialized foam mattresses, gel cushions, and heel protectors are designed to provide support without compromising blood flow.
Skin assessment and care involve routine checks for any signs of redness, breakdown, or irritation on the heels. Keeping the skin clean and moisturized minimizes friction and helps maintain skin integrity, which is essential in preventing ulcers.
Nutritional support plays a critical role in skin health; a well-balanced diet that includes sufficient fluids, vitamins, and minerals helps maintain skin elasticity and resilience. This nutritional foundation is vital for healing and preventing any pressure-related injuries.
Education and training for caregivers and patients are fundamental in promoting awareness of pressure ulcer prevention strategies. By understanding the importance of mobility, skin care, and the use of appropriate devices, everyone involved can contribute to reducing the incidence of heel pressure ulcers.
How Can Heel Pressure Ulcers Be Managed Successfully at Home?
The best treatment for heel pressure ulcers at home involves a combination of proper wound care, pressure relief, and nutrition.
- Regular Wound Cleaning: Keeping the ulcer clean is crucial to prevent infection and promote healing. Use a saline solution or a gentle cleanser recommended by a healthcare provider, and avoid harsh soaps that can irritate the skin.
- Moisture Management: Maintaining a moist wound environment can enhance healing. Use appropriate dressings that retain moisture, such as hydrocolloids or foam dressings, which can protect the ulcer while allowing for gas exchange.
- Pressure Relief Techniques: Relieving pressure on the affected heel is essential to prevent further damage. Utilize cushions, heel protectors, or specialized mattresses that redistribute weight away from the ulcer.
- Nutrition and Hydration: Adequate nutrition supports healing, so a diet rich in proteins, vitamins, and minerals is important. Ensure proper hydration as well, as it helps maintain skin elasticity and overall health.
- Regular Position Changes: Changing positions frequently helps to alleviate pressure on the heel. Aim to shift weight every 30 minutes to an hour if sitting, or use turning schedules if bedridden.
- Monitoring for Infection: Keep an eye out for signs of infection, such as increased redness, swelling, or discharge. If any of these symptoms occur, contact a healthcare professional for assessment and possible intervention.
- Consultation with Healthcare Providers: Regular check-ins with a healthcare provider can ensure that the treatment plan is effective. They can provide tailored advice and adjustments based on the healing progress of the ulcer.
